This page provides information about the tonsils and surgery of the tonsils including reasons surgery may be recommended, risks associated with surgery, and postoperative instructions.
What are tonsils and adenoids and why are they removed?
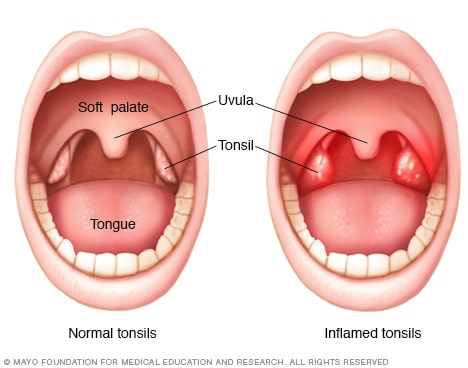
The Tonsils are located in the throat near the base of the tongue. The Adenoids are located in the back of the nose. The tonsils & adenoids are part of our immune system but only a small part. Patients who have their tonsils removed still have a strong immune system and do not have any more illnesses than people who have their tonsils.
The most common reasons for surgery recommendation to remove tonsils and/or adenoids are:
- Recurrent infections
- Chronic infections/inflammation
- Peritonsillar abscess
- Enlarged tonsils
- Asymmetric size
- Tonsil stones and bad breath
Tonsillitis is inflammation of the tonsils. The inflammation results in sore throat, difficulty and pain with swallowing, fever and frequently changes of the appearance of the tonsils. It can be cause by viral and bacterial infections and the majority will resolve with time, even without antibiotic treatment. When tonsils are infected with a type of bacteria known as Group A Strep, antibiotics are given to prevent complications of the heart and kidneys. When infections occur frequently or are more severe or chronic in nature surgery to remove the tonsils and adenoids may be beneficial.
Chronic tonsillitis is longer term inflammation and it occurs in some individuals causing chronic sore throat, halitosis, difficulty or pain with swallowing, tonsillitis, and persistently tender cervical nodes. Sometimes patients have mild low grade inflammation that leads to more mild but prolonged symptoms, this may occur with or without stones. This is termed chronic tonsillitis.
Tonsilloliths are small white concretions that look and feel like small stones. These result from debris collecting in the surface of the tonsils. These can cause irritation and contribute to bad breath (halitosis). Sometimes patients have chronic irritation resulting from these collections. Most patients do not require surgery for this condition but when symptoms are more severe or chronic or conservative measures have failed surgery may be recommended.
Peritonsillar abscess is a serious infection that results when a pocket of infected fluid accumulates near the tonsil. Individuals often have severe throat pain, fever, drooling, foul breath, trismus (difficulty opening the mouth), and voice changes.
Tonsillar hypertrophy is abnormal enlargement of the tonsil tissue. Hypertrophy may cause problems related to the size of the tissue and problems may include difficulty swallowing, easy gagging, loud snoring or obstruction of the airway (apnea). Large tonsils are rarely the sole cause of snoring or sleep related problems in adults. The significance of the enlargement can sometimes be difficult to establish. Some patients with large tonsils have no problems related to the enlargement and do not need surgery. If symptoms related to the increased size are significant then surgery can be performed to remove the tonsils.
Asymmetric tonsils results when the right and left tonsils have notably different size. Usually this is a benign problem but if there is concern or suspicion that the asymmetry is resulting from a more serious problem your doctor may recommend removal.
Surgery
Tonsillectomy is surgery to removal the tonsils. It is performed by an ears, nose, and throat surgeon in the operating room while the patient is under general anesthesia. The goal of surgery is to remove the tissue so that it won’t continue to cause problems from infections or enlargement. The tonsil is removed from a pocket leaving a small raw area which heals over 1-2 weeks. The area remains very sensitive and mild to severe pain is typical for 10 to 14 days. The tonsil may be removed by itself or at the same time as the adenoids. Adenoidectomy is uncommon in adults but if any concerns are present the adenoid tissue may be removed also. Most of the time patients can go home the same day.
Risks of Surgery: Risks are uncommon and include, but are not limited to the following:
Anesthesia risks. These are related to the process of general anesthesia are extremely rare, your child will be carefully monitored during the procedure. If you have a personal or family history of anesthesia related problems or a history of bleeding problems let your physician know.
Bleeding. This can occur during or after the procedure. It may occur up to 10 days after surgery. Frequently the bleeding stops on its own, sometimes it can be treated in the emergency room, but sometimes the patient will have to go back to the operating room for treatment (especially if they are young).
Dehydration. Since it is painful to swallow, sometimes patients will avoid drinking and become dehydrated. This may require a trip back into the ER or hospital and re-hydration with IV fluids.
Damage to the teeth, lips, and gums. Surgery is performed in the mouth and rarely the structures of the mouth can be injured from surgical instruments
Voice change. Theoretical but very uncommon
Velopharyngeal insufficiency (VPI). Normally the palate closes against the back of the throat to prevent food and fluids from entering the nasal cavity. Occasionally after adenoidectomy, the palate has to readjust and patients may have temporary reflux of food and liquids into their nose. Permanent problems are very rare.
Wound problems. These can include scaring, infection, abnormal healing.
Residual disease or recurrent problems. Occasionally problems that we are trying to treat persist.
Discharge Instructions for Throat Surgery
DRINKING –Drinking plenty of fluids is key to a healthy recovery. Starting immediately after surgery, patients may have fluids such as water or apple juice. Make an effort to drink every hour during waking hours for the first two days after surgery. Contact your physician if there are signs of dehydration. Caffeinated drinks in excess should be avoided because they will cause the patients to lose the fluids. Some patients experience nausea and vomiting after the surgery. This usually occurs within the first 24 hours and resolves on its own after the effects of anesthesia wear off.
EATING –A regular but soft diet is best after surgery. Soft foods like pasta, rice, eggs are better tolerated; avoid tough/crispy/crunchy foods. The sooner the patient eats and chews, the quicker the recovery. Tonsillectomy patients may be reluctant to eat because of throat pain and some temporary weight loss may occur.
PAIN –Throat pain and/or ear pain is common after tonsillectomy and it can take up to 2 weeks for you to feel better. Ear pain frequently occurs between the 3rd and 7th days and results from special nerve connections.
Following tonsillectomy give regular doses of pain medications 4 to 5 times a day for a week. Medicine will take 30 minutes to start working. Sleeping will be tough. Anti-inflammatory medications such as Motrin, Advil, Ibuprofen, Aleve, and Naproxen Sodium are also frequently used and help reduce pain and inflammation and can be alternated with the other pain medications. Your Surgeon will have prescribed a Pain Medication and it should be used as directed. Further measures to decrease throat discomfort are numbing throat spray of Cepacol Dual Action and Chloroseptic, drinking plenty of cool/cold beverages, especially water, cool compresses to the neck, ice chips or the use of chewing gum. You swallow 5 times a minute and each and every time will hurt. TAKE THE PAIN MEDICINE AND HYDRATE!
BLEEDING –You should have no bleeding after returning home. There is a bleeding risk after surgery for 2 weeks. If there is blood streaked mucous or saliva try drinking icy slushy liquids and/or gargle with ice chips mixed with water. If this does not stop the bleeding after 30 minutes, call our office during duty hours from M-F at 406-752-8330 to receive further instructions. If you notice any bright red blood, or dark black emesis (vomiting after the first three days) go to the nearest ER.
FEVER –It is normal for patients to run a fever between 99 and 1O1 degrees for the first few days following tonsillectomy. Fever is worsened by a poor fluid intake producing dehydration.
ACTIVITY –It is advisable to rest at home for the first 48 hours. During this time patients should be up and walking. The more you move around, the sooner you will start to feel better. Activity may be increased slowly, with a return to work after normal eating and drinking resumes, and pain medication is no longer required. Travel on airplanes or far away from a medical facility is not recommended for two weeks following surgery. Vigorous physical activity should be avoided for 14 days following tonsil surgery.
BAD BREATH -Bad breath is quite common. This results from a white to yellowish membrane that forms in the throat in the region of the tonsil surgery. Bad breath may be improved by gargling a mild salt water solution. This may be made by adding 1/2 teaspoon of table salt to 8oz. of warm tap water. The membrane sloughs off during healing between the 5th and 10th days postoperatively and when this occurs the patient may spit up some bloody mucous.
These are some common medications prescribed after surgery.
- Tylenol Aceteminophen
Use: Tylenol is an excellent medication used for mild to moderate pain
Instructions: Adults, Adolescents, and Children >= 12 years: 325—650 mg by mouth (PO) every 4—6 hours, as needed. Alternatively, 1000 mg PO, 2—4 times per day can be given.
Precautions: Do not exceed 1 g/dose or 4 g/day. - Naprosyn / Naproxen / Aleve
Use: Naprosyn is an anti-inflammatory medication that provides pain relief. It is used for mild to moderate pain
Instructions: Adults: 500 mg PO twice daily. The dose may be increased to two 500mg tablets in the morning and one at night when a higher level of analgesic/anti-inflammatory activity is required.
Precautions: Do not with other anti-inflammatory medications such as Motrin. - Motrin / Ibuprofen
Use: Motrin is used for mild to moderate pain
Instructions: Adults: 400—800 mg PO 3—4 times a day as needed.
Precautions: Doses exceeding 50 mg/kg/day are not recommended. Do not take with other anti-inflammatory medications. - Tylenol and Oxycodone combination: Percocet / Roxicet
Use: Medication combinations of Tylenol and oxycodone (narcotic) are used for moderate to severe pain.
Instructions: Oral dosage:
Adults: 1—2 tablets or capsules (5 mg of oxycodone) by mouth (PO) every 6 hours as needed. It may be necessary to exceed the usual dosage recommendation (i.e., give every 4 hours) in cases of severe pain. You may take one Tylenol and one Percocet tablet for mild to moderate pain
Precautions: Do not drive while taking this medication. Maximum acetaminophen dose is 4 g/day. Do not take full doses of Tylenol and Percocet as you will exceed the maximum acetaminophen dose. - Steroids: Decadron(Dexamethasone) Prednisone / Medrol
Use: Steroids reduce inflammation and swelling and are used after some procedures
Instructions: See specific prescription. Steroids are often tapered meaning the starting dose is higher and the dose is gradually decreased.
Precautions: Steroids can cause indigestion and mood changes. Let your physician know if you have any past history of gastric ulcers, TB, or other issues. - Mouth Wash
Frequent a combination mouth wash (Diphenhydramine/Maalox/Lidocaine) is given to provide topical relief. It usually only last a short while. Follow directions provided if this medication is given. Peridex is a peroxide containing mouth wash that helps clean your mouth but may sting. It can be diluted with water if necessary. - Anti-nausea medication Zofran
If you have a history of nausea or vomiting after surgery you may be given some medication to take as needed.