What is GERD?
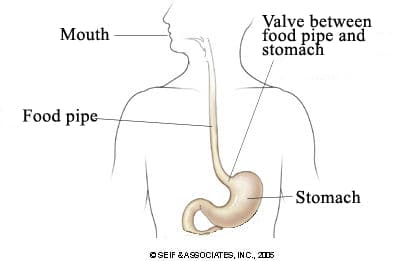
Gastroesophageal reflux disease, often referred to as GERD, occurs when acid from the stomach backs up into the esophagus. Normally, food travels from the mouth, down through the esophagus and into the stomach. A ring of muscle at the bottom of the esophagus, the lower esophageal sphincter (LES), contracts to keep the acidic contents of the stomach from “refluxing” or coming back up into the esophagus. In those who have GERD, the LES does not close properly, allowing acid and other contents of the digestive tract to move up-to “reflux”-the esophagus.
When stomach acid touches the sensitive tissue lining the esophagus and throat, it causes a reaction similar to squirting lemon juice in your eye. This is why GERD is often characterized by the burning sensation known as heartburn.
In some cases, reflux can be silent, with no heartburn or other symptoms until a problem arises. Almost all individuals have experienced reflux (GER), but the disease (GERD) occurs when reflux happens often over a long period of time.
What is LPR?
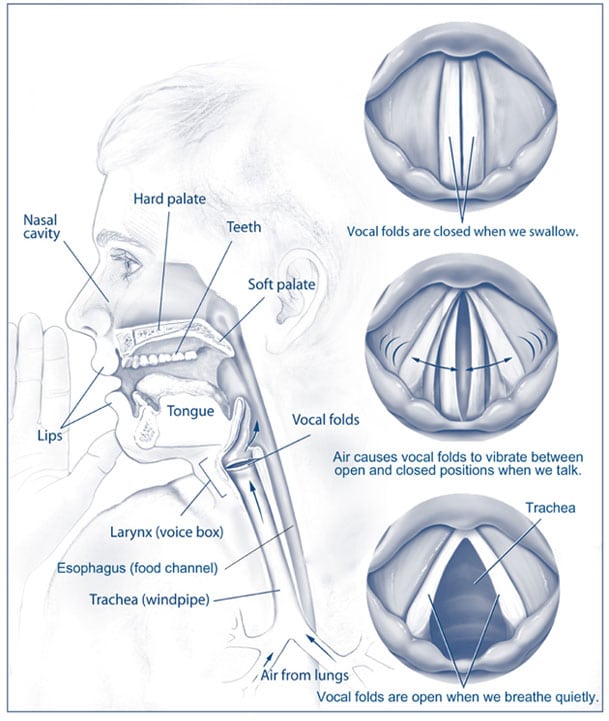
During gastroesophageal reflux, the contents of the stomach and upper digestive tract may reflux all the way up the esophagus, beyond the upper esophageal sphincter (a ring of muscle at the top of the esophagus), and into the back of the throat and possibly the back of the nasal airway. This is known as laryngopharyngeal reflux (LPR), which can affect anyone. Adults with LPR often complain that the back of their throat has a bitter taste, a sensation of burning, or something feels “stuck.” Some patients have hoarseness, difficulty swallowing, throat clearing, and difficulty with the sensation of drainage from the back of the nose (“postnasal drip”). Some may have difficulty breathing if the voice box is affected. Many patients with LPR do not experience classic heartburn.
In infants and children, LPR may cause breathing problems such as: cough, hoarseness, stridor (noisy breathing), croup, asthma, sleep-disordered breathing, feeding difficulty (spitting up), turning blue (cyanosis), aspiration, pauses in breathing (apnea), apparent life threatening event (ALTE), and even a severe deficiency in growth. Proper treatment of LPR, especially in children, is critical.
What are the symptoms of GERD and LPR?
The symptoms of GERD and LPR fall on a spectrum and may include persistent heartburn, acid regurgitation, indigestion, nausea, hoarseness in the morning, or trouble swallowing, feeling of something stuck, sense of post nasal drip, need to clear the throat, a dry cough, or a feeling there is a collection of mucous in the back of the throat. The symptoms vary and can be subtle.
While GERD and LPR may occur together, patients can also have GERD alone (without LPR) or LPR alone (without GERD). If you experience any symptoms on a regular basis (twice a week or more), then you may have GERD or LPR. For proper diagnosis and treatment, you should be evaluated by your primary care doctor or an otolaryngologist—head and neck surgeon (ENT doctor).
Who gets GERD or LPR?
Women, men, infants, and children can all have GERD or LPR. These disorders may result from physical causes or lifestyle factors. Physical causes can include a malfunctioning or abnormal lower esophageal sphincter muscle (LES), hiatal hernia, abnormal esophageal contractions, and slow emptying of the stomach. Lifestyle factors include diet (chocolate, citrus, fatty foods, spices), destructive habits (overeating, alcohol and tobacco abuse) and even pregnancy. Young children experience GERD and LPR due to the developmental immaturity of both the upper and lower esophageal sphincters. It should also be noted that some patients are just more susceptible to injury from reflux than others. A given amount of refluxed material in one patient may cause very different symptoms in other patients.
Unfortunately, GERD and LPR are often overlooked in infants and children, leading to repeated vomiting, coughing in GERD, and airway and respiratory problems in LPR, such as sore throat and ear infections. Most infants grow out of GERD or LPR by the end of their first year, but the problems that resulted from the GERD or LPR may persist.
What role does an ear, nose, and throat specialist have in treating GERD and LPR?
A gastroenterologist, a specialist in treating gastrointestinal orders, will often provide initial treatment for GERD. But there are ear, nose, and throat problems that are caused by reflux reaching beyond the esophagus, such as hoarseness, laryngeal nodules in singers, croup, airway stenosis (narrowing), swallowing difficulties, throat pain, and sinus infections. These problems require an otolaryngologist—head and neck surgeon, or a specialist who has extensive experience with the tools that diagnose GERD and LPR. They treat many of the complications of GERD and LPR, including: sinus and ear infections, throat and laryngeal inflammation and lesions, as well as a change in the esophageal lining called Barrett’s esophagus, a serious complication that can lead to cancer.
Your primary care physician or pediatrician will often refer a case of LPR to an otolaryngologist head and neck surgeon for evaluation, diagnosis, and treatment.
How are GERD and LPR diagnosed and treated?
GERD and LPR can be diagnosed or evaluated by a physical examination and the patient’s response to a trial of treatment with medication. Other tests that may be needed include an endoscopic examination, biopsy, x-ray, 24 hour pH probe with or without impedance testing, esophageal motility testing (manometry), and emptying studies of the stomach. Endoscopic examinations can often be performed in your ENT’s office, or may require some form of sedation and occasionally anesthesia.
Most people with GERD or LPR respond favorably to a combination of lifestyle changes and medication. Medications that could be prescribed include antacids, histamine antagonists, proton pump inhibitors, pro-motility drugs, and foam barrier medications. Some of these products are now available over the counter and do not require a prescription.
Children and adults who fail medical treatment or have anatomical abnormalities may require surgical intervention. Such treatment includes fundoplication, a procedure where a part of the stomach is wrapped around the lower esophagus to tighten the LES, and endoscopy, where hand stitches or a laser are used to make the LES tighter.
Adult lifestyle changes to prevent GERD and LPR
Avoid eating and drinking within two to three hours prior to bed time.
- Do not drink alcohol
- Eat small meals and slowly
- Limit problem foods:
- Caffeine and Carbonated drinks
- Chocolate
- Peppermint
- Tomato
- Citrus fruits
- Fatty and fried foods
- Lose weight
- Lose weight
- Quit smoking
- Wear loose clothing
Laryngopharyngeal Reflux / Reflux Laryngitis Protocol
In some people, irritating acidic stomach juices may flow backward out of the stomach and into the esophagus and throat, voice box and lungs. This causes irritation, decreased sensation, and muscle spasms in the throat. Some of the symptoms include: cough, burning or soreness, hoarseness, throat clearing, excess mucous, bitter taste, bad breath, and a sensation of a lump in the throat. Many people with laryngopharyngeal reflux and reflux laryngitis do not experience classic heartburn as a common symptom of their reflux disease. Most people with classic GERD (gastro esophageal reflux disease) do experience heartburn!
The following instructions are designed to help neutralize the stomach acid, reduce the production of acid, and prevent acid from coming up the esophagus and into the larynx and throat. You should use as many of the suggestions as you need to get relief. If these
measures do not help, or if your symptoms get worse, you should let the physician know about it. Items 1 through 4 are particularly important.
1.) Sleep with the head of your bed elevated. There are two good ways to accomplish this.
a. Place a brick, block, or something under the headboard of your bed to raise the head of the bed about 5-6 inches. This will create a gentle slant of the entire bed helping gravity to keep the acid in your stomach. This mild elevation is generally not even noticed after a few nights.

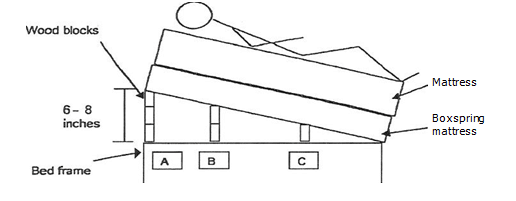
b. You can also elevate the box spring instead of the headboard. The best way to do this is: Place a series of “steps” under the box spring to create an incline as shown in the diagram. Try to elevate the head to a height of 6-8 inches. If the frame is strong enough, bricks, wood or cinder blocks can be placed under the legs at the head of the bed. This graduated method of elevation of the head of the bed helps to keep the mattress stable.
Sleeping on several pillows is not advised. It creates further compression on your abdomen by bending you at the waist (similar to “sit ups”), and promotes reflux episodes while you are sleeping.
2.) Do not eat for 3 or 4 hours before lying down to sleep.
3.) Exercise (including aerobic exercise, weight lifting, singing, and public speaking) on an empty stomach or wait 2-3 hours after eating and drinking before performing such activities. Activities and exercises which require lifting, bending, stooping, etc., should be minimized, especially while your acute symptoms are present.
4.) Alcohol, tobacco, and caffeine are irritants to the esophagus and should be avoided, especially in the evening. Alcohol and caffeine also promote reflux episodes and may stimulate stomach secretions.
5.) Diet restrictions help control symptoms. A small bland diet divided into multiple small feedings is recommended. You should avoid highly seasoned foods, fatty foods, and foods rich in dairy products, acidic foods (tomatoes, lemons, etc.), onions, and peppermint. Experiment with one food at a time to determine which foods and/or seasonings worsen your symptoms. Care should be taken to chew food thoroughly.
6.) If you are over-weight, you should lose weight. Sometimes weight loss of as little as 5-10 pounds can have a tremendous effect on the occurrence of reflux episodes. Ask us for a referral to a clinical dietician for assistance.
7.) Wearing clothing that fits tightly across the midsection of the body should be avoided (for example, girdles, tight belts, corsets, etc.).
8.) Maintaining a relaxed attitude in your activities helps to reduce symptoms.
9.) Recent evidence suggests that chewing sugarless gum, especially bicarbonate gum, helps control reflux. If there are no dental reasons why you cannot chew gum, it is worth checking the effects of gum chewing for about a half an hour after meals, or at other times when reflux is troublesome. Chewing two sticks is more effective than chewing only one.